This four-part article series provides an in-depth review of wisdom teeth, what they are and what the procedure and recovery process involves in their removal.
Common Problems Associated with Wisdom Teeth
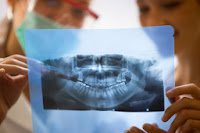
 Wisdom teeth misalignment: "It's not uncommon for the third molars to emerge at an angle away from or towards the second molars”. “We’ve also had patients whose wisdom teeth have emerged from the gums horizontally! This can apply pressure to the entire dental arch, causing overcrowding. Badly aligned wisdom teeth can also damage the jawbone, the adjacent teeth and the nerves, causing much pain for the patient.”
Wisdom teeth misalignment: "It's not uncommon for the third molars to emerge at an angle away from or towards the second molars”. “We’ve also had patients whose wisdom teeth have emerged from the gums horizontally! This can apply pressure to the entire dental arch, causing overcrowding. Badly aligned wisdom teeth can also damage the jawbone, the adjacent teeth and the nerves, causing much pain for the patient.” Wisdom Teeth Removal: What Does the Procedure Entail?


 “Treating TMD is far more complex than simply taking a course of prescribed medication,” explains a Silver Spring cosmetic dentist. “The kind of treatment we recommend also depends substantially on how severe a patient’s condition is. Usually, the best approach is to begin with conservative therapy, which should appease the symptoms. If the symptoms persist, surgery may ultimately be required.”
“Treating TMD is far more complex than simply taking a course of prescribed medication,” explains a Silver Spring cosmetic dentist. “The kind of treatment we recommend also depends substantially on how severe a patient’s condition is. Usually, the best approach is to begin with conservative therapy, which should appease the symptoms. If the symptoms persist, surgery may ultimately be required.”  Adjust Your Diet: Refrain from eating hard, crunchy foods (hard candy, crisps, raw vegetables, ice, caramels) and foods that require you to stretch open your mouth to fit. Rather, stick to a softer diet (yogurt, soup, cooked vegetables, mashed potato, fish, etc.) for a few weeks or as recommended by your dentist. Cut smaller bites and chew gently. You’re trying to rest the TMJ and give the swelling and inflammation a chance to subside.
Adjust Your Diet: Refrain from eating hard, crunchy foods (hard candy, crisps, raw vegetables, ice, caramels) and foods that require you to stretch open your mouth to fit. Rather, stick to a softer diet (yogurt, soup, cooked vegetables, mashed potato, fish, etc.) for a few weeks or as recommended by your dentist. Cut smaller bites and chew gently. You’re trying to rest the TMJ and give the swelling and inflammation a chance to subside.  You may have TMD if you have noticed one or more of the following symptoms:
You may have TMD if you have noticed one or more of the following symptoms:  As it was previously explained, the exact cause of TMD is not always clear, which can make it tricky to identify. Many patients are led to believe that they have other medical problems, since the symptoms of TMD manifest in a great number of areas on the body and not only the joint. As such, they might not seek the help of a dentist in Silver Spring MD. Additionally, there are a host of other conditions (gum disease, sinus problems and toothache) that come hand-in-hand with similar symptoms, so diagnosis needs to be done carefully and precisely.
As it was previously explained, the exact cause of TMD is not always clear, which can make it tricky to identify. Many patients are led to believe that they have other medical problems, since the symptoms of TMD manifest in a great number of areas on the body and not only the joint. As such, they might not seek the help of a dentist in Silver Spring MD. Additionally, there are a host of other conditions (gum disease, sinus problems and toothache) that come hand-in-hand with similar symptoms, so diagnosis needs to be done carefully and precisely. 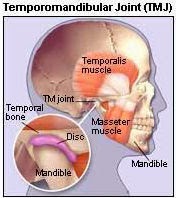 “Temporomandibular disorders (TMD) refer to a suite of problems that affect the articulating joint of the jawbone,” explains the Silver Spring dentist. “The temporomandibular joint (TMJ) is where the mandible (lower jaw) meets the skull at the temple (hence the name of the joint). If you put two fingers against your face right in front of either ear, you’ll feel the joint articulating when you open and close your mouth.”
“Temporomandibular disorders (TMD) refer to a suite of problems that affect the articulating joint of the jawbone,” explains the Silver Spring dentist. “The temporomandibular joint (TMJ) is where the mandible (lower jaw) meets the skull at the temple (hence the name of the joint). If you put two fingers against your face right in front of either ear, you’ll feel the joint articulating when you open and close your mouth.” 
 There are a number of approaches a skilled dentist can take to treating gum recession. First and foremost, he or she will want to diagnose the cause of the recession and provide treatment so that it ceases. In most cases, gum recession is caused by oral bacterial infection, so treating the infection will put an end to the southward (or skyward) march of the gum line. If the cosmetic dentist in Silver Spring MD determines that your case isn’t too far advanced, he or she will typically prescribe a deep cleaning of the affected area beneath the gum line and the polishing or “planing” of the tooth roots to make it difficult for bacteria to re-infect it. Planing and root scaling is often accompanied by a course of anti-biotic medication.
There are a number of approaches a skilled dentist can take to treating gum recession. First and foremost, he or she will want to diagnose the cause of the recession and provide treatment so that it ceases. In most cases, gum recession is caused by oral bacterial infection, so treating the infection will put an end to the southward (or skyward) march of the gum line. If the cosmetic dentist in Silver Spring MD determines that your case isn’t too far advanced, he or she will typically prescribe a deep cleaning of the affected area beneath the gum line and the polishing or “planing” of the tooth roots to make it difficult for bacteria to re-infect it. Planing and root scaling is often accompanied by a course of anti-biotic medication. In advanced cases, the cosmetic dentist in Silver Spring may opt to perform surgery to eliminate diseased tissue, bacteria and other calculus from the entire tooth structure. He or she will then reverse the damage done to the gums (as far as possible) using the following procedures:
In advanced cases, the cosmetic dentist in Silver Spring may opt to perform surgery to eliminate diseased tissue, bacteria and other calculus from the entire tooth structure. He or she will then reverse the damage done to the gums (as far as possible) using the following procedures: “When the gums recede and pull away from the crowns of the teeth, the roots become exposed to the food you eat, bacteria and abrasive actions, such as toothbrushing,” explains the dental implants specialist in Maryland. “The difference between your tooth roots and crowns is that the latter is specifically protected against general wear-and-tear by dental enamel. So, when the roots become exposed, they can easily become damaged and decayed.
“When the gums recede and pull away from the crowns of the teeth, the roots become exposed to the food you eat, bacteria and abrasive actions, such as toothbrushing,” explains the dental implants specialist in Maryland. “The difference between your tooth roots and crowns is that the latter is specifically protected against general wear-and-tear by dental enamel. So, when the roots become exposed, they can easily become damaged and decayed. If your dentist determines that the extent of gum recession is too far advanced and the pockets between your tooth roots and gums too deep, you may be referred to a periodontist for surgery to eliminate diseased tissue and repair the damage done to your gums. This may involve procedures such as pocket depth reduction, soft tissue grafting and regeneration. These will be fully explained in Part 4 of this article series, but for now, the orthodontist in Silver Spring MD provides us with a list of gum recession prevention tips...
If your dentist determines that the extent of gum recession is too far advanced and the pockets between your tooth roots and gums too deep, you may be referred to a periodontist for surgery to eliminate diseased tissue and repair the damage done to your gums. This may involve procedures such as pocket depth reduction, soft tissue grafting and regeneration. These will be fully explained in Part 4 of this article series, but for now, the orthodontist in Silver Spring MD provides us with a list of gum recession prevention tips...



 RSS Feed
RSS Feed
