|
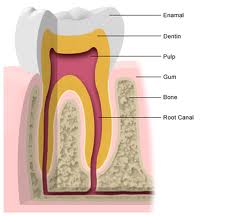
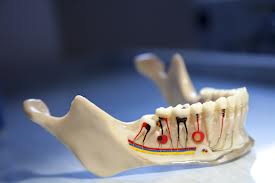
This three-part article series takes an in-depth look at root canal therapy: what it is, why it’s necessary and what patients can expect from the procedure. Little else strikes fear in the heart of the patients quite like the words “root canal” do. This procedure has such a bad reputation that the expression “was more painful than a root canal” has become a popular English language idiom! But, is this procedure deserving of such a reputation? What exactly IS root canal therapy anyway? And what necessitates this procedure? In this three-part article series, the dentist in Silver Spring MD speaks to us about root canal therapy and why it could be the only thing that stands between you and a gappy smile! The Anatomy of a Tooth  Technically, a root canal is not actually a procedure... root canal therapy, also referred to as endodontic treatment, is. Root canals are the tiny spaces inside the roots of your teeth. They, together with the pulp chamber (see image below) house the living “guts” of the tooth, including the blood vessels, nerves and connective tissue: collectively referred to as the “pulp”. Root canal therapy becomes necessary when these delicate tissues become infected. Usually, the body deals quite effectively with diseased tissue by sloughing it off or expelling it in some form or manner. In the case of your teeth, however, this pulp is trapped within the exceptionally hard casing of the tooth. So, when bacteria infiltrate the protective dental enamel and infect the pulp, the health of the entire tooth becomes critically endangered. There’s simply no way the body can deal effectively with the infection. This leaves the patient with two options: (1) root canal therapy or (2) tooth extraction. Either way, action needs to be taken or else the tooth will decay excruciatingly in the mouth and eventually fall out on its own. Having a decaying tooth in your mouth is not only terribly unpleasant, but it can actually make you sick. What is Root Canal Therapy?  “Root canal therapy involves the elimination of diseased tissue inside an infected tooth,” explains the dentist in Silver Spring MD. “We do this by drilling a hole in the top of the tooth and removing all of the pulp from the inner tooth chamber and the root canals. Once the insides of the tooth have been thoroughly cleaned and sterilized, we fill it with “gutta percha” - a rubber compound - and a special sealer paste, which will prevent bacteria from getting inside the tooth again. We then cap the tooth, usually with a durable and aesthetic ceramic crown so that the tooth appears as though nothing ever happened to it.” The procedure is, of course, a little more detailed than this and we shall provide a blow-by-blow account of what goes on during a root canal in part 3 of this article series. Stay Tuned for Part 2 Stay tuned for the second installment of this three-part article series on root canal therapy. In our next article, the dentist in Silver Spring MD will provide us with a little more detail on what can cause a patient to require such a procedure in the first place and how we can recognize the various signs and symptoms of an inner tooth infection.
0 Comments
Leave a Reply. |
AuthorOur multi-dentist approach means we can provide you with the best options in a single comprehensive plan, and then implement them without you having to leave your comfortable dental chair. When you're finished, you'll get one consolidated statement for each family member and one representative who can answer any questions you may have. Archives
March 2014
Categories
All
|